🩺Hypertension in Pregnancy: Diagnosis and Management – NICE Guideline Summary
Overview
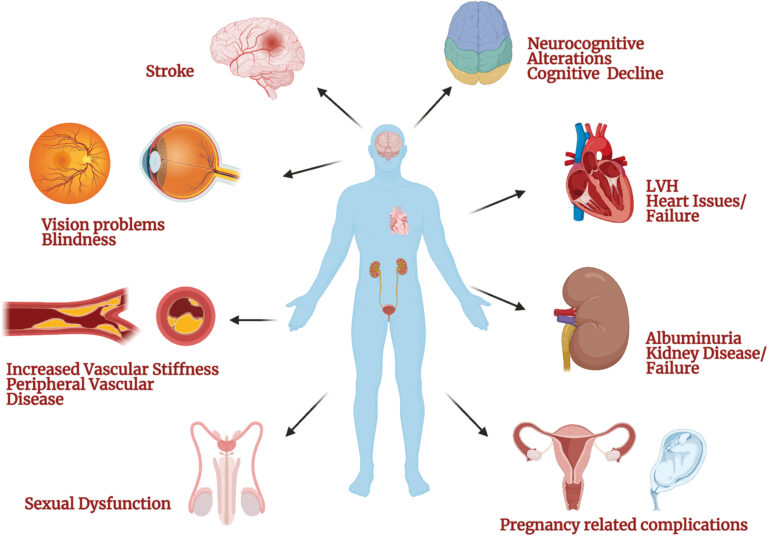
Hypertensive disorders are among the most common medical complications of pregnancy and a major cause of maternal and perinatal morbidity and mortality worldwide. They include chronic hypertension, gestational hypertension, and pre-eclampsia. Early recognition, appropriate monitoring, and timely intervention are critical to reduce risks to both mother and baby. NICE NG133 (2019, updated 2023) provides evidence-based recommendations for diagnosis, prevention, and management.
Definitions
Chronic hypertension is hypertension present before pregnancy or diagnosed before 20 weeks’ gestation. Gestational hypertension is new-onset hypertension (≥140/90 mmHg) arising after 20 weeks without proteinuria or systemic involvement. Pre-eclampsia is hypertension after 20 weeks associated with either proteinuria, maternal organ dysfunction (such as renal, hepatic, neurological or haematological), or uteroplacental dysfunction such as fetal growth restriction. Severe hypertension is defined as systolic ≥160 mmHg or diastolic ≥110 mmHg.
Risk Assessment and Prevention
At booking, women should be assessed for risk factors for pre-eclampsia including first pregnancy, previous history of pre-eclampsia, multiple pregnancy, chronic hypertension, diabetes, renal disease, autoimmune disease, obesity, or advanced maternal age. Women at high risk should be advised to take low-dose aspirin (75–150 mg daily) from 12 weeks until delivery. Lifestyle advice such as healthy diet, exercise, and avoidance of excessive weight gain is also recommended.
Diagnosis and Monitoring
Blood pressure should be measured with a validated device, in both arms at the first visit, and confirmed by repeat readings. Ambulatory or home monitoring may help in borderline cases. Investigations at diagnosis include urinalysis with protein:creatinine ratio (PCR) or albumin:creatinine ratio (ACR), renal and liver function tests, platelet count, and sometimes uric acid. Fetal assessment should include ultrasound for growth, amniotic fluid volume, and Dopplers, with CTG or non-stress testing as indicated. Women with severe hypertension, features of pre-eclampsia, or evidence of maternal or fetal compromise should be referred to specialist obstetric care.
Management in Pregnancy
For non-severe hypertension, the target blood pressure is 135/85 mmHg. For severe hypertension (≥160/110 mmHg), treatment should be initiated immediately. First-line antihypertensive choices are labetalol, nifedipine, or methyldopa. In acute severe cases, IV labetalol, IV hydralazine, or oral nifedipine may be used. ACE inhibitors, ARBs, and renin inhibitors are contraindicated in pregnancy. Maternal surveillance includes regular BP checks, enquiry about symptoms such as headache, visual disturbance, or epigastric pain, and repeat blood and urine tests. Fetal surveillance involves serial growth scans, Doppler studies, and cardiotocography if needed. Admission is often required in severe cases.
Timing and Mode of Delivery
For women with chronic or gestational hypertension, delivery is usually recommended from 37 weeks if maternal and fetal condition is stable. For pre-eclampsia, delivery should be considered at 37 weeks or earlier if disease is severe, maternal or fetal compromise develops, or BP remains uncontrolled. Expectant management before 34 weeks may be appropriate in specialist units with close monitoring and corticosteroids for fetal lung maturity. Mode of delivery is determined by obstetric indications, fetal status, and cervical favourability.
Postnatal and Long-Term Care
Blood pressure often peaks in the first 48 hours postpartum, so careful monitoring is essential. Antihypertensive treatment should be continued and tapered as appropriate. Women should be counselled about their increased long-term risk of hypertension, cardiovascular disease, and recurrence in future pregnancies. Pre-pregnancy counselling should include optimisation of BP and use of aspirin in subsequent pregnancies.
Exam Pearls (RCOG Focused)
Key definition: Pre-eclampsia = hypertension ≥20 weeks + proteinuria or maternal/fetal organ dysfunction (proteinuria is no longer essential).
Target BP: 135/85 mmHg (exam favourite).
Severe hypertension threshold: 160/110 mmHg → immediate treatment.
First-line drug: Labetalol; alternatives nifedipine, methyldopa.
Avoid ACEi/ARBs (teratogenic).
Seizure prophylaxis: Magnesium sulfate for severe pre-eclampsia/eclampsia.
Delivery timing: At 37 weeks for pre-eclampsia, earlier if severe/unstable.
Postpartum: Avoid methyldopa due to depression risk; BP rises after delivery, so monitoring is essential.
Recurrence: Prior pre-eclampsia increases risk in future pregnancies — aspirin from 12 weeks reduces risk.
High-yield numbers:
Miscarriage risk after CVS ~0.5–1% (for context in genetics questions).
Aspirin dose: 75–150 mg daily.
Severe hypertension = ≥160/110.
