Management of syphilis in pregnancy and children: Updated Summary of BASHH Guidelines 2024
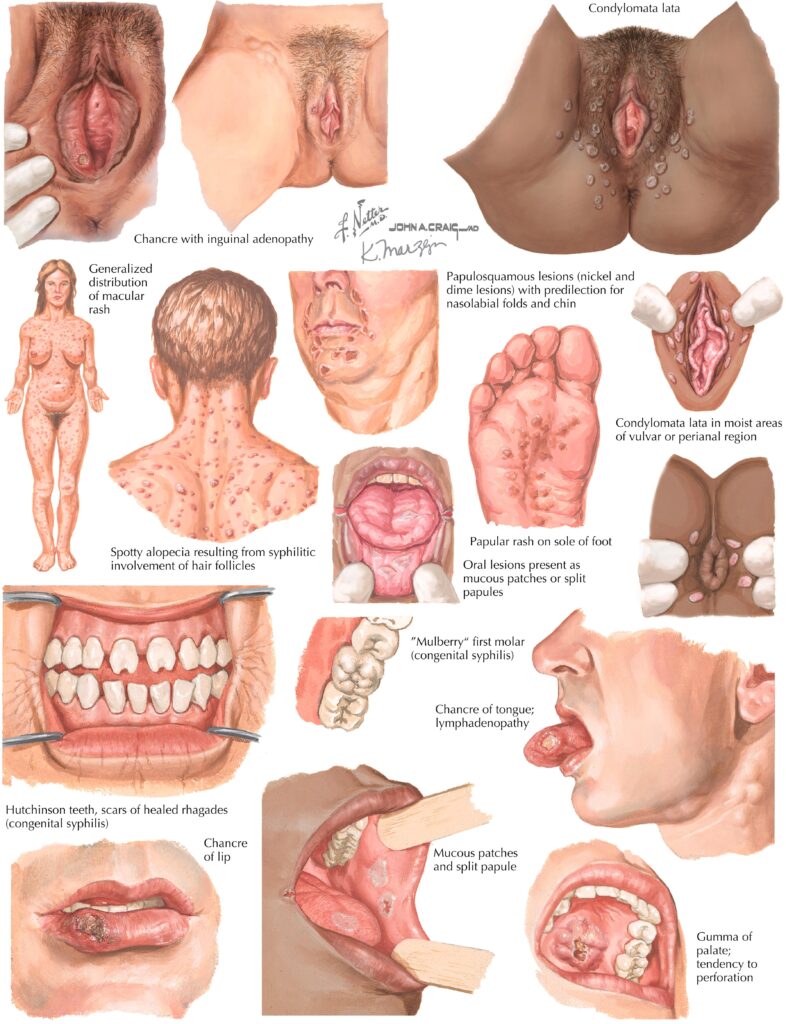
Here are the most important practical recommendations from the guideline and related UK antenatal policy (as implemented via the national antenatal screening programme) — vital for exams and for clinical reasoning:
• Universal antenatal screening
All pregnant women should be offered serological testing for syphilis at their first antenatal visit (booking bloods). This is standard practice in the UK.
A positive screening test does not necessarily mean active infection — it may indicate past treated syphilis, false‑positive, or latent disease. Hence referral to specialist sexual health services (SHS) for full assessment is mandatory for all positive screens.
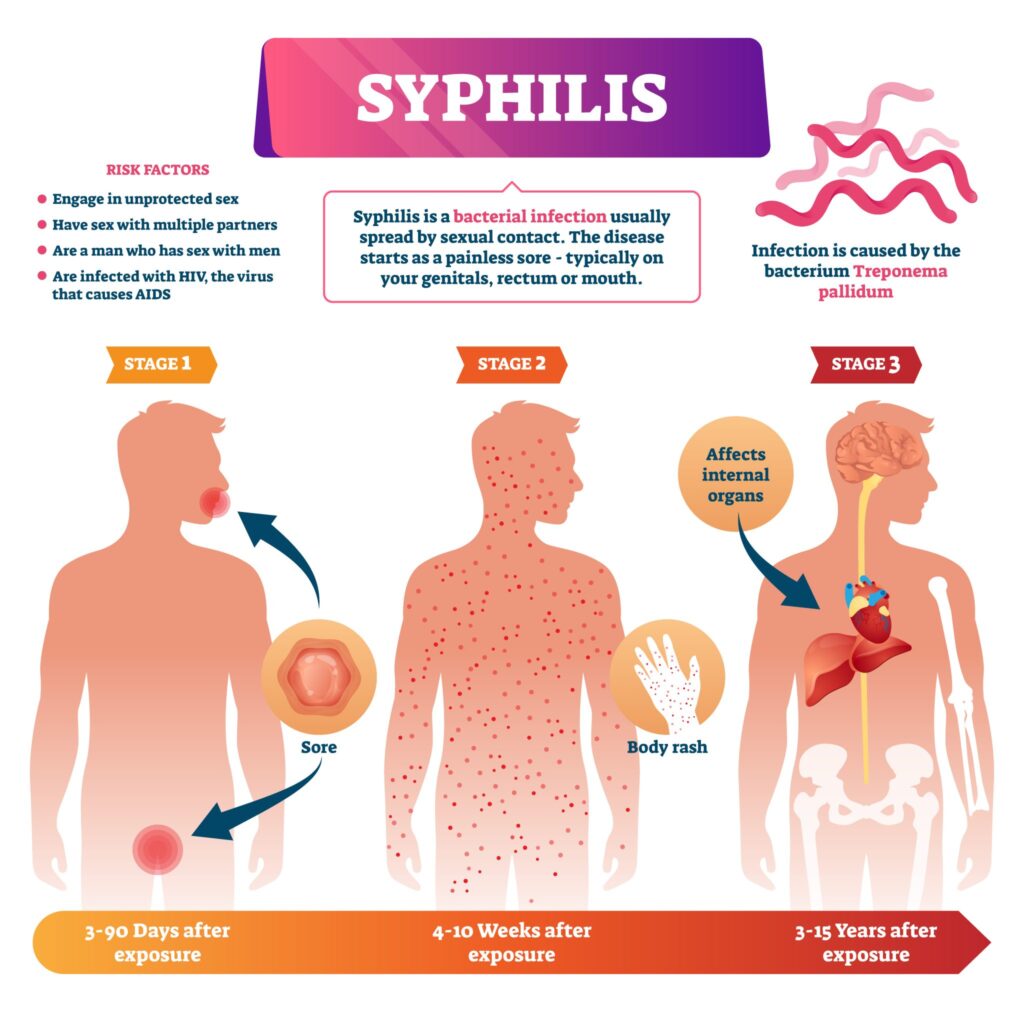 • Prompt referral and timely assessment
• Prompt referral and timely assessment
Once a confirmed positive screen is identified, the antenatal screening team should inform the woman, offer counselling, and refer to SHS within 5 working days.
SHS should assess the woman within 10 working days of referral. Assessment includes review of serology, clinical history, prior treatment, risk factors, and need for treatment.
A “birth‑plan” must be completed for all women with a confirmed positive screen (even if, after assessment, no treatment is required). This ensures neonatal teams are aware at delivery. GOV.UK+1
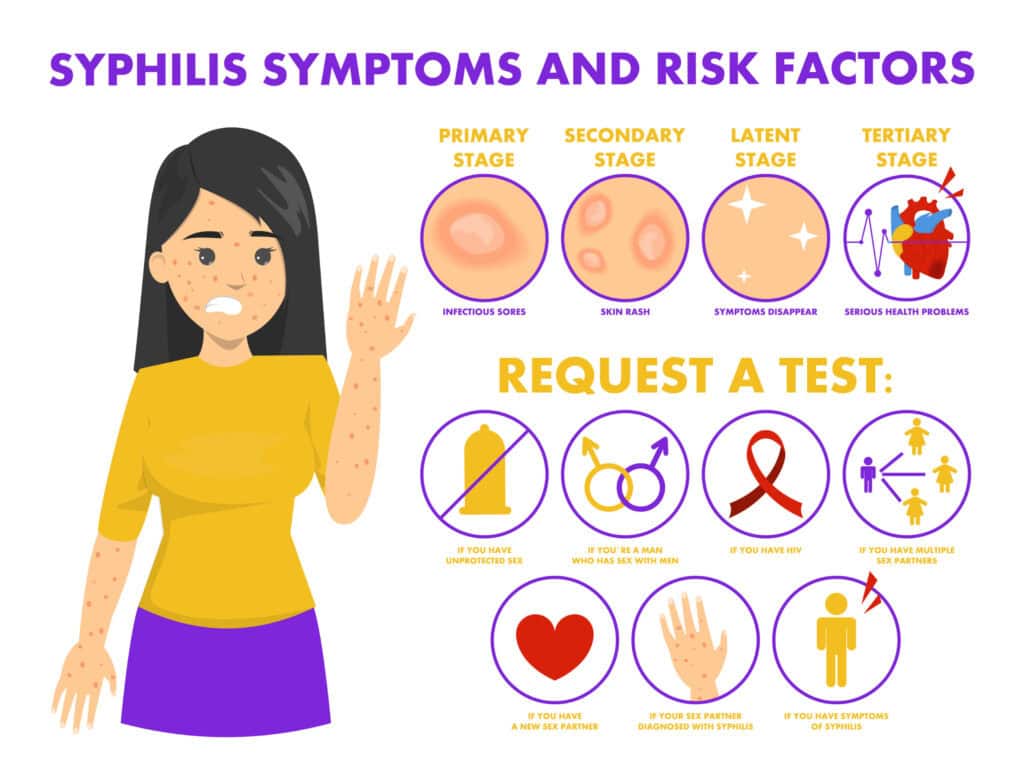 • Treatment — when indicated & penicillin remains first‑line
• Treatment — when indicated & penicillin remains first‑line
If maternal syphilis requires treatment in pregnancy, injectable penicillin (e.g. benzathine penicillin) is the recommended therapy, because it crosses the placenta and treats both mother and fetus.
Timely treatment is vital: untreated or inadequately treated maternal syphilis carries high risk of adverse fetal/neonatal outcomes — miscarriage, stillbirth, neonatal death, congenital infection.
After maternal treatment, follow‑up and documentation must be completed, including notification to relevant screening surveillance services.
• Neonatal / Infant management & follow‑up
All infants born to treated mothers must have a neonatal review at birth, including full physical examination and syphilis serology.
Outpatient follow-up for the infant is also required (often at 3 months), even if no obvious signs at birth.
If maternal serology is due to false-positive, or syphilis was treated before pregnancy with documented adequate treatment — risk to neonate is minimal; birth‑plan should reflect that to avoid unnecessary interventions.
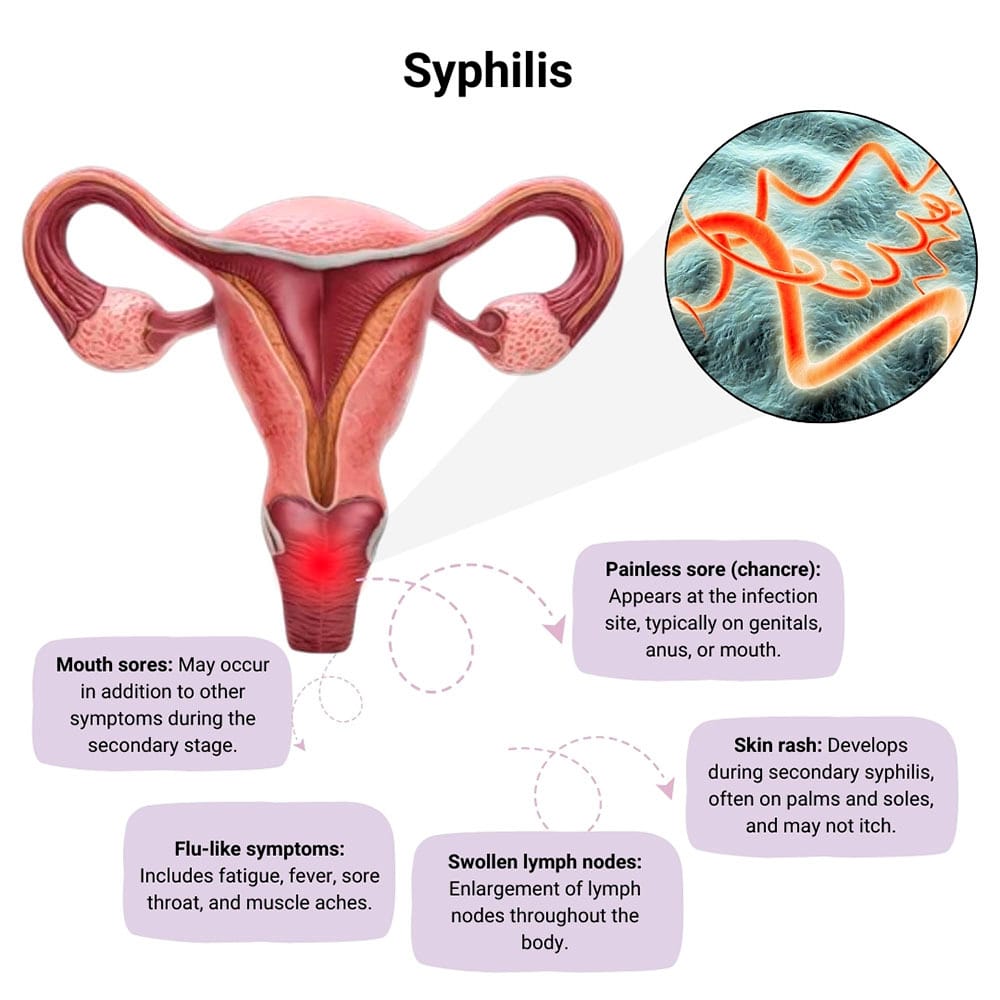 • Prevention of reinfection & partner management
• Prevention of reinfection & partner management
Partner(s)/sexual contacts should be tested and treated if positive — to avoid reinfection of mother (and risk to fetus) later in pregnancy. UKHSA Research Portal+1
Sexual health promotion, counselling and risk assessment are integral — not just treating the infection.
⚠️ Why this matters — Key Clinical / Exam Points & Pitfalls
From an exam and clinical‑practice perspective (especially in obstetrics/gynecology):
False positives are common. A positive serological screen does not equal active syphilis — relying on just the screening result (without assessment) may lead to overtreatment or undue stress. The guideline mandates referral and assessment before treatment decisions.
Penicillin remains essential. Since penicillin crosses placenta and treats fetus — alternate antibiotics (e.g. oral macrolides) are suboptimal, especially for preventing congenital syphilis. Missing penicillin (stock out, allergy) may result in fetal infection.
Time-critical treatment. Delay in treatment — especially if first detected late in pregnancy — increases risk of fetal loss, stillbirth, congenital syphilis. Hence, timely referral & treatment (after screening) is vital.
Multidisciplinary care is essential. Management involves antenatal services, sexual-health services, obstetrics, neonatal/pediatrics for infant follow-up — highlighting why solely obstetric‑based guidance (e.g. from RCOG) may be insufficient; specialist guideline (BASHH) is necessary.
Importance of documentation & birth planning. For safe delivery and neonatal care — even if mother doesn’t require treatment. For exam questions, knowing that a “birth plan” + neonatal alert + infant serology are recommended is vital.
Prevention of reinfection & public health angle. Screening, partner notification, health education — emphasising that syphilis in pregnancy isn’t just a biomedical issue but also a public health one.
🎯 What to Remember for Exam (or Clinical Recall)
If you have a short-answer or viva during an RCOG‑style exam and are asked about syphilis in pregnancy, here are the minimal key points from BASHH 2024 you should mention:
Universal antenatal syphilis screening at booking (first visit).
Positive screen → refer to sexual‑health services for full assessment; don’t treat without confirmatory assessment.
Penicillin (benzathine) is first-line; treat mother to prevent congenital syphilis.
Neonatal management: physical exam + serology at birth + follow up (e.g. 3 months).
Birth‑plan for all positive-screened women, even if no maternal treatment needed.
Partner testing/treatment + health education to prevent reinfection.
If asked for “complications of untreated maternal syphilis”: mention miscarriage, stillbirth, neonatal death, congenital syphilis, preterm birth, low birth weight, neonatal morbidity (jaundice, anaemia, neurologic problems). (These align with data on vertical transmission risks.)
🧠 Why There’s No RCOG Green‑Top but BASHH is More Relevant
As you had previously noted, RCOG does not have a dedicated Green‑top guideline on syphilis in pregnancy.
Management of syphilis in pregnancy requires integration of obstetrics, sexual health (STI), microbiology, neonatal care — so a specialist STI guideline from BASHH (with broad stakeholder input) is more suited.
BASHH 2024 guideline fills this gap: giving clear standardised UK‑wide recommendations for pregnancy + neonates.
Hence, for exam or clinical use, if asked “How to manage syphilis in pregnancy,” it’s appropriate (and often expected) to refer to BASHH 2024 guidance, even in context of obstetric practice.
BASHH UK guidelines for the management of syphilis in pregnancy and children 2024 click below
