PCOS and Fertility: Best Treatments That Work in 2025

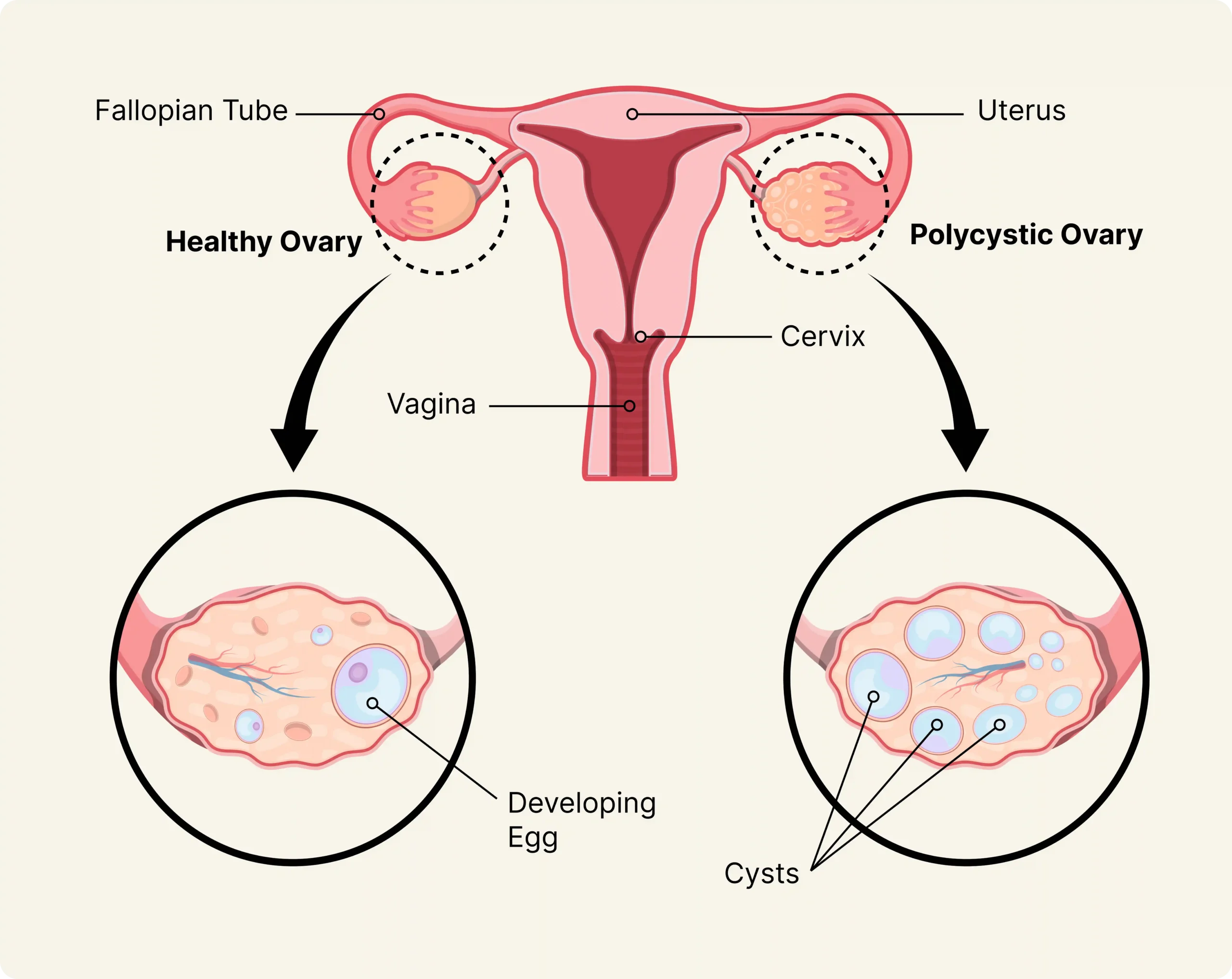
What is PCOS?
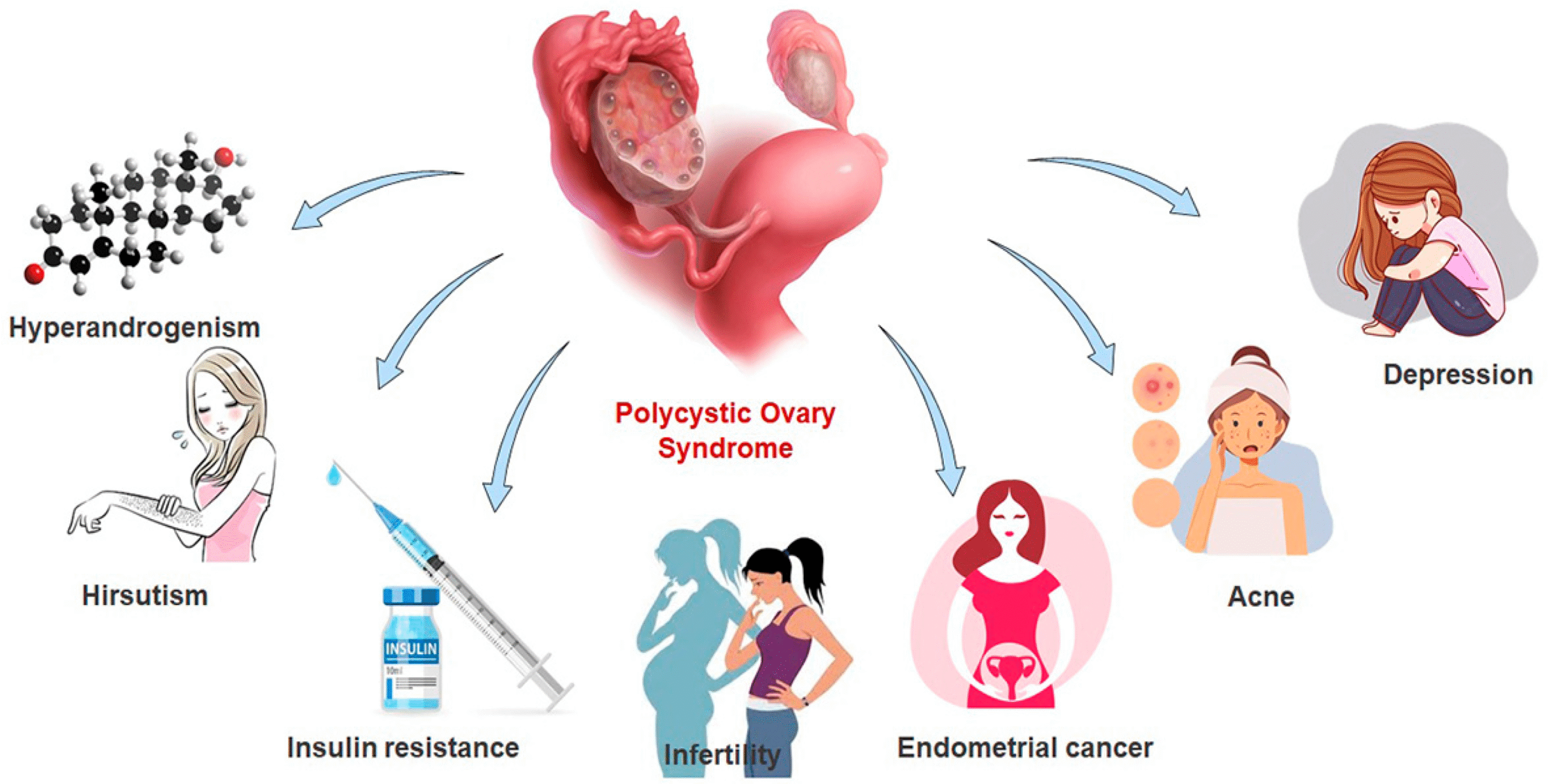
Polycystic Ovary Syndrome (PCOS) is one of the most common hormonal disorders affecting women of reproductive age. It is caused by an imbalance in reproductive hormones (especially excess androgens and insulin resistance) that disrupts normal ovulation.
Women with PCOS often experience irregular or absent periods, acne, excess hair growth, weight gain, and difficulty conceiving. Studies suggest that PCOS affects 1 in 10 women worldwide, making it a leading cause of infertility.
How Does PCOS Affect Fertility?
Fertility problems in PCOS occur mainly due to:
Irregular Ovulation: Eggs are not released regularly, reducing chances of conception.
Poor Egg Quality: Hormonal imbalance can affect egg maturation.
Insulin Resistance: High insulin levels increase androgens (male hormones), which further disrupt ovulation.
Endometrial Issues: The uterine lining may not prepare properly for implantation.
This combination makes it harder for women with PCOS to get pregnant naturally without medical support.
Best Treatments for PCOS and Fertility in 2025
1. Lifestyle Modifications (First-line treatment)
Weight Management: Even a 5–10% weight loss can restore ovulation in overweight women.
Diet: Low glycemic index (GI) diet, high in lean protein, fiber, and whole grains helps control insulin resistance.
Exercise: 30–45 minutes of moderate physical activity (walking, yoga, strength training) improves insulin sensitivity and hormone balance.
2. Medications for Ovulation Induction
Letrozole (Femara): Now considered the first-line medication for inducing ovulation in women with PCOS.
Clomiphene Citrate: Traditionally used, still effective for some women.
Metformin: Improves insulin resistance, can restore cycles and enhance ovulation when combined with other treatments.
3. Assisted Reproductive Techniques (ART)
If oral medications fail, doctors may recommend:
Ovarian Drilling (laparoscopic surgery): Reduces androgen levels and can improve ovulation.
Intrauterine Insemination (IUI): Sperm is placed directly into the uterus to increase chances of conception.
In Vitro Fertilization (IVF): Especially effective if other infertility factors exist or if ovulation medications fail.
4. New and Emerging Treatments in 2025
Inositol Supplements (Myo-Inositol & D-Chiro Inositol): Shown to improve insulin resistance and ovulation rates.
GLP-1 Receptor Agonists (for weight loss & insulin resistance): Being studied for women with PCOS struggling with obesity.
Personalized IVF Protocols: Advances in reproductive technology allow tailoring ovarian stimulation to PCOS patients, reducing risks of ovarian hyperstimulation.
Tips for Women Trying to Conceive with PCOS
Track ovulation with apps or ovulation kits.
Maintain a balanced lifestyle with sleep, stress management, and exercise.
Work with a fertility specialist early — don’t wait too long if cycles remain irregular.
Consider combining medical treatment + lifestyle changes for the best outcomes.

How to Conceive with PCOS
PCOS is a major cause of infertility, but with the right management, most women can conceive successfully. In 2025, the combination of lifestyle modification, effective medications like Letrozole, and advanced fertility treatments (IVF, IUI) is offering renewed hope to women worldwide.
If you’re trying to get pregnant with PCOS, consult a gynecologist or fertility specialist to create a personalized plan — because every woman’s journey is unique.

What Happens if PCOS is Not Controlled?
1. Infertility & Pregnancy Complications
Persistent anovulation (no egg release) → infertility.
Higher risk of miscarriage.
Increased pregnancy complications such as gestational diabetes, preeclampsia, and preterm birth.
2. Metabolic Disorders
Insulin Resistance → Type 2 Diabetes: Up to 50–70% of women with PCOS develop insulin resistance.
Obesity: Uncontrolled weight gain worsens symptoms.
High Cholesterol & Hypertension: Increases cardiovascular risk.
3. Endometrial Cancer Risk
Women with long-term irregular or absent periods may have endometrial hyperplasia (thickened uterine lining).
This increases risk of endometrial cancer if untreated.
4. Cardiovascular Disease
Higher rates of heart disease, stroke, and metabolic syndrome.
Increased atherosclerosis (plaque in arteries) risk due to chronic inflammation and high cholesterol.
5. Hormonal & Cosmetic Concerns
Severe acne, hirsutism (excess hair growth), male-pattern baldness.
These can cause psychological stress, low self-esteem, anxiety, and depression.
6. Mental Health Issues
Higher incidence of anxiety, depression, and eating disorders.
Sleep problems (including sleep apnea) are more common.
✅ In summary:
If PCOS is not controlled, it can progress beyond fertility problems and lead to diabetes, heart disease, endometrial cancer, and serious emotional health challenges. Early diagnosis, lifestyle management, and medical treatment are essential.